ROSA offers hope to epilepsy patients
At 20 years old, a young woman who suffered from refractory epilepsy feels as if she has been born again. For the bulk of her childhood, Lindsay Snyder struggled to have a normal life and was suffering from as many as four seizures a day. Now, thanks to a team of expert neurosurgeons at Memorial Hermann, a specialized robotic service (ROSA), and a dedicated team of neurologists, Lindsay is reclaiming her independence and ability to live a healthy, normal life.
Before her first seizure at the age of nine, Lindsay loved cheerleading and performing stunts for her squad. Then her seizures started, and Lindsay felt increasingly frustrated knowing that she was missing out on so many things. As the epilepsy worsened, she had to give up playing sports, a sacrifice that was especially difficult for her as the daughter of Texas A&M University Defensive Coordinator Mark Snyder. At 16, when most of her peers were learning how to drive, Lindsay couldn’t because of her illness. By her senior year of high school, she was told she was in danger of not graduating on time because of how much school she had missed.
“I can’t explain how difficult it was,” Lindsay said. “It was awful. I couldn’t do anything by myself. I spent most of my days in the nurse’s office at school. When I had a seizure at school, the EMS was required to come and so they came almost every single day. I missed so much class that I had to go in front of the school board and explain to them why I wasn’t in class.”
For years Lindsay and her family struggled to find the right medical treatment for her illness. Doctors ran several MRIs, EEGs and tests on Lindsay, but the results failed to reveal a specific cause or the brain region where the horrible seizures she was experiencing originated. Some doctors thought she was faking her seizures because she was stressed or desired attention.
Yet Lindsay and her family knew the seizures were real and weren’t responsive to therapy or medication. Fortunately, during one of her visits to the doctor, a nurse informed Lindsay that there was something out there that could help her. The nurse told Lindsay about her personal struggle with epilepsy and how she had been cured with a new, highly specialized surgery.
From that moment on, Lindsay was determined to have surgery. Yet she was still young and finding a hospital that could perform the surgery wasn’t an easy task. Even today, there are only a few sites in the world that would consider surgery in a case such as hers. Fortunately for her, in June of 2013 the Memorial Hermann Mischer Neuroscience Institute at the Texas Medical Center became one of three sites in the United States to offer a life-changing procedure using robotic stereoelectroencephalography (SEEG).
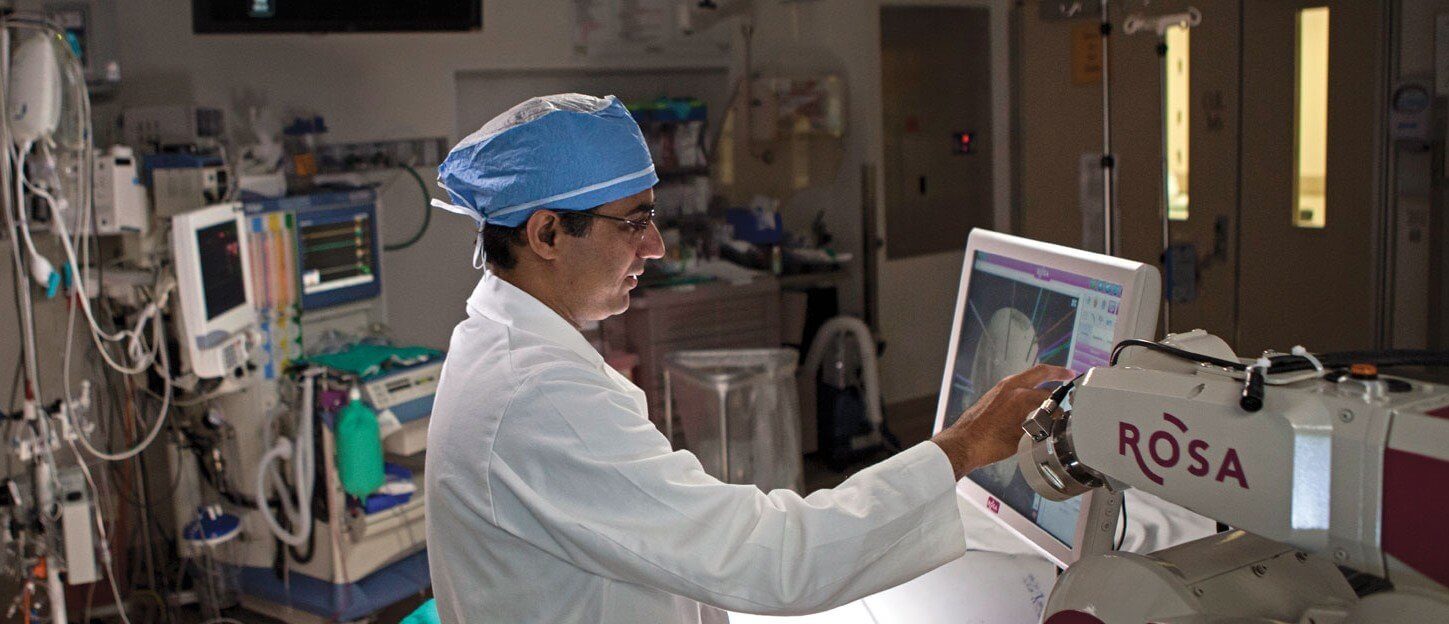
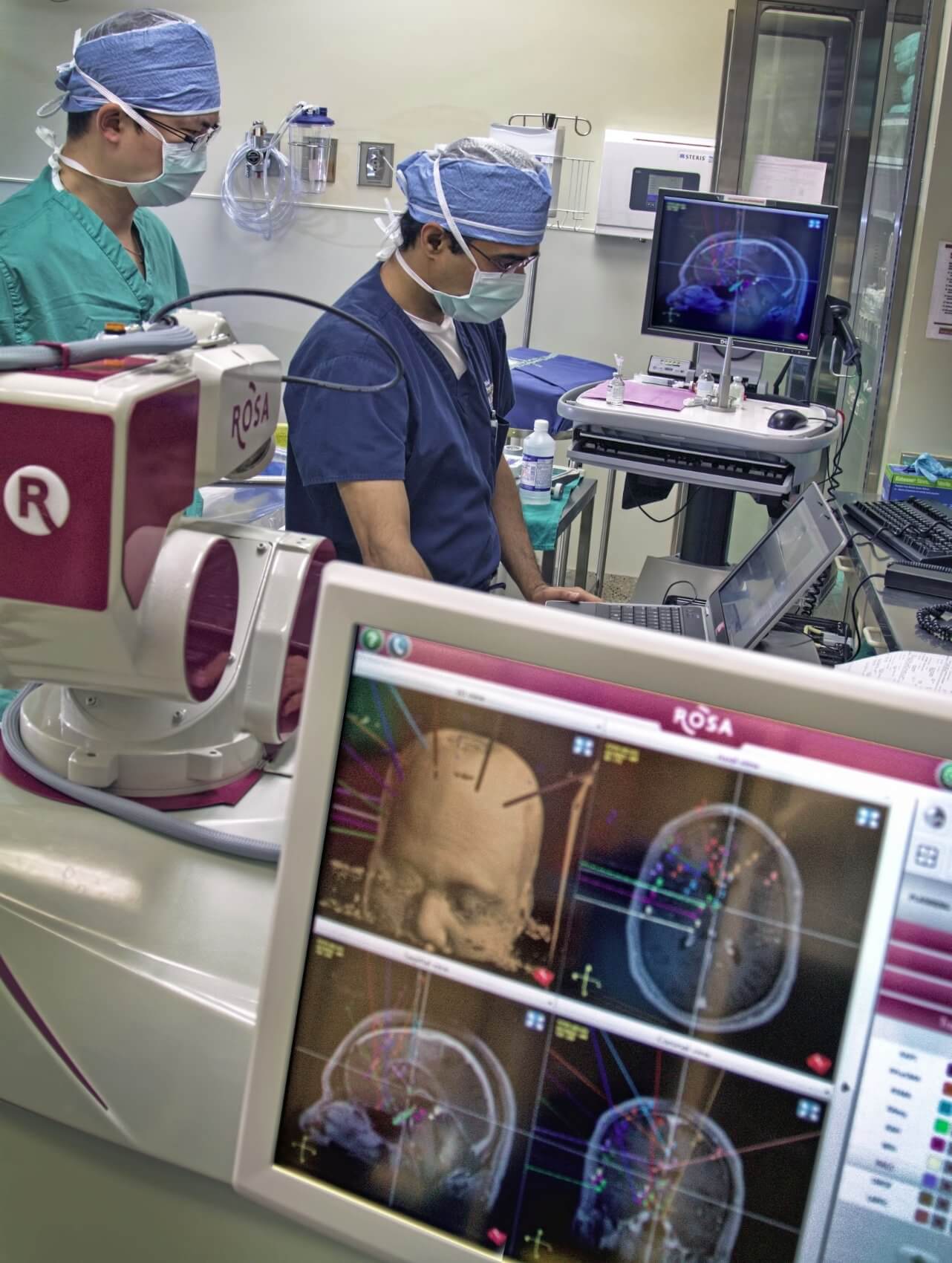
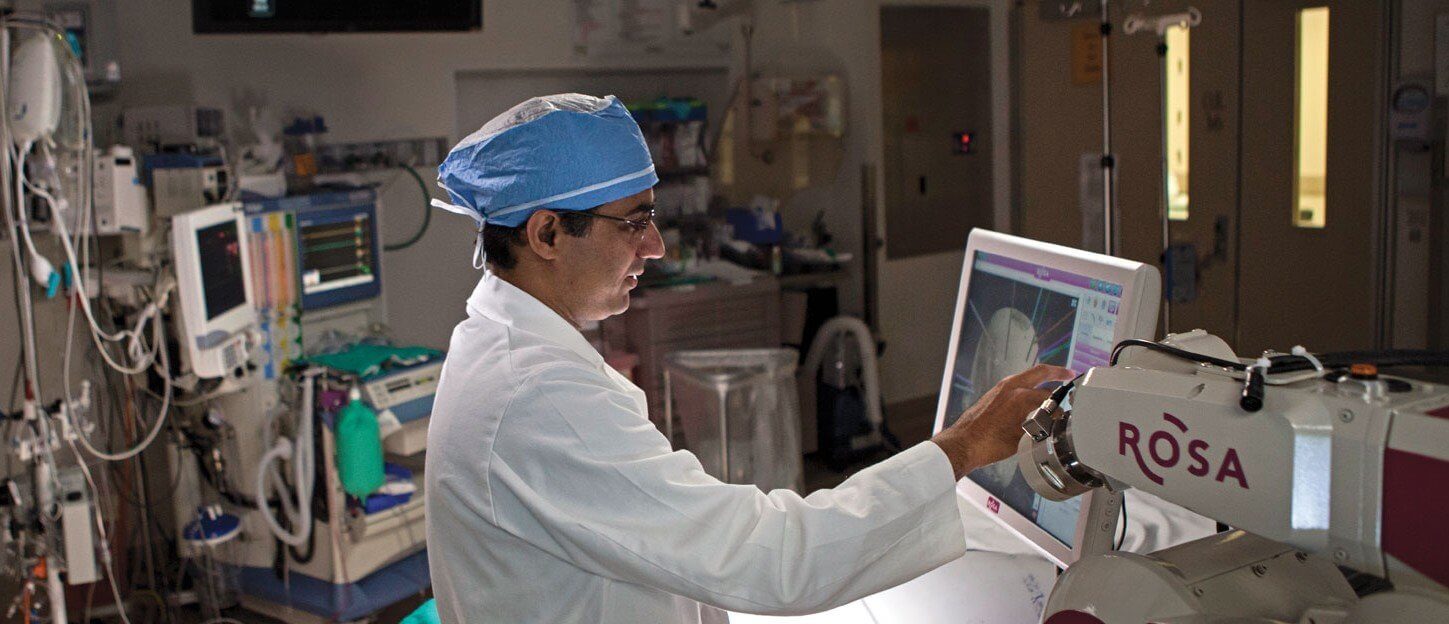
Stereoelectroencephalography is a 3-D approach to localizing seizures using very thin electrodes, placed with great precision, into specific brain regions. The ROSA stereotactic robot is used to place these electrodes accurately and has been successful in localizing the seizure focus in patients like Lindsay who suffer from severe epilepsy that cannot be treated with medication. Through advanced technology, ROSA can pinpoint exact areas of epileptic activity that are not always easily detectable. Then doctors can devise a plan to operate on the affected parts. Prior to robotic SEEG, neurosurgeons had to perform invasive craniotomies that cut into large portions of the skull in order to access the brain, posing a greater risk for human error. Now, by using the robot, neurosurgeons can deliver faster and more precise results in a less invasive manner. The electrodes are thin—measuring at .8mm thick—and operations can be completed in as little as two hours.
“In our desire to help our patient population, we have devised an approach that allows us to place electrodes with both great precision and speed in this innovative approach that allows us to evaluate patients with epilepsy who we had not been able to help in the past,” said Nitin Tandon, M.D., the neurosurgeon who performed Lindsay’s operation. Tandon is director of epilepsy surgery at Memorial Hermann Mischer Neuroscience Institute at the Texas Medical Center and associate professor in the Department of Neurosurgery at The University of Texas Health Science Center at Houston (UTHealth) Medical School. “If we had seen Lindsay two years ago, we may not have had a feasible option for her non-lesional, poorly lateralizable frontal lobe epilepsy,” he said. “But using robotic SEEG, we were able to localize the epilepsy and then plan for a curative operation using ROSA.”
In August of 2013, Lindsay became one of the first patients at Memorial Hermann to benefit from the ROSA robot. Since then, she has been seizure-free and is quickly moving forward with her life, accomplishing everything she had been desperately wanting to do.
“I was really nervous when I was going in,” Lindsay said. “I kept saying I wasn’t going to get nervous, but when I got in the surgery room, I started freaking out. When I got home my head was a bit sore and I had stitches and staples in my head, but after a few months, my life became amazing. I’m driving. I just got a job. I’m in college. I’m living my life the way I’ve always wanted to.”
“It was such a heartbreaking thing to watch every day for 10 years, to see our precious daughter suffer and just literally get worse, day by day, before our eyes,” said Beth Snyder, Lindsay’s mother. “So to have her where she is now—a normal college girl who can go and do things that weren’t possible for so many years—I just can’t even put into words how overwhelming it is.”
In just over one year, Tandon and his team at Memorial Hermann Mischer Neuroscience Institute have performed over 40 operations using the ROSA robot. Tandon feels especially grateful knowing he can provide this unique, life-changing operation for patients who previously were unable to manage their epilepsy.
“Epilepsy is a disease that really affects people’s lives in terrible ways,” Tandon said. “I’ve had so many people tell me the impact that it has had on their lives. Not being able to be left alone or take a bath without their parents or spouse being concerned because they could drown. Not being able to drive, which obviously has a huge impact on their social ability, economic abilities, and being unable to get to work, hold a job. I’ve had many patients with children who are desperate now to have surgery so that they can take their child to the park or drop them off at school. Being able to give people their life back is really gratifying. The single most rewarding thing we do as caregivers is to cure someone of a chronic debilitating illness.”
At Memorial Hermann and UTHealth, neurosurgeons like Tandon work hand-in-hand with the epilepsy neurologists to provide patients with comprehensive care and total support. Melissa Thomas, M.D., Lindsay’s epilepsy neurologist, and Giri Kalamangalam, M.D., work closely with Tandon to devise the precise SEEG plan that would most likely help localize the epilepsy in each individual case. Additionally, the hospital has a 12-bed Epilepsy Monitoring Unit, a magnetoencephalography program, a dedicated team approach that extends beyond neurosurgeons and neurologists to neuropsychologists, neuroradiologists and neuropathologists, and a support group to connect patients and families who are affected by the disease. Memorial Hermann also sponsors reunions for patients who have undergone surgery or epilepsy treatment. Each year the opportunities and technologies for patients with epilepsy continue to grow.
“There are so many things that we can do as caregivers to take away the stigma of the disease,” said Tandon. “One of the things that I, or people like Lindsay, can do is to help people understand that epilepsy is not something they need to be ashamed of. It’s just like having asthma, diabetes or something else that could be life-threatening in certain situations. Except in this case, it affects the brain and people seem to respond to that with more fear. Over the last ten years that I have been at Memorial Hermann, we have created an epilepsy program that is larger, more innovative and more comprehensive than anything in this region. We’re very happy to be in the Texas Medical Center and to be able to bring more attention to our city and medical center. It is, in many ways, a work of passion. It’s a lot of work to get people better, but it’s very gratifying—indeed it’s a privilege to be able to do what we do.”