Alzheimer’s disease and the long goodbye

In the crowded clubhouse of her New Orleans apartment complex, Judie Gabler noticed a dashing young man stagger through the door with two friends. It was Friday, Oct. 15, 1971—close to midnight—and Gabler’s apartment building was throwing a Las Vegas-themed party for tenants. The man had “the most beautiful eyes” and a smolder that made him look like an actor right out of Hollywood’s Golden Age.
Kenny Tidwell, who was almost 29 and recently divorced, was a former college football star who played for Louisiana Tech University and graduated with a degree in accounting. He lived just a few blocks from Judie and had been working as a scout for Getty Oil before being promoted to a landman.
Judie and her friends taught Kenny and his friends how to shoot craps that night. Around 3 a.m., Kenny turned to Judie and said, “I have tickets to the Saints game Sunday. Want to go?”
Judie paused. She already had season tickets, but she was undeniably smitten.
“I was crazy about him right off the bat,” Judie said. Two days later, Kenny and Judie watched the New Orleans Saints beat the Dallas Cowboys 24-14. It was the first of many dates.
“He was adamant he was never getting married again, would never own another house, never mow another lawn, never have another kid,” Judie said. “Never, never, never, never.”
She heard that speech from him often, each version bringing tears to her eyes. But on June 23, 1975, Kenny popped the question.
He brought her to Antoine’s in the French Quarter of New Orleans, her favorite restaurant, where they dined on crabmeat ravigote, filet mignon with marchand du vin sauce, a soufflé and drank a bottle of Châteauneuf-du-Pape.
Even after nearly 44 years of marriage, Judie can recall that night in great detail.

Judie and Kenny Tidwell on their wedding day on Oct. 24, 1975.
But Kenny doesn’t remember anything.
“Did I go?” he asked, earnestly, after listening to Judie reminisce about their courtship.
“You must have. You gave me the ring,” she quipped. It was a magical proposal, by all accounts, but those memories and so many others have been stolen from Kenny by Alzheimer’s disease.
Confusion, frustration
Kenny was diagnosed with Alzheimer’s in January 2013 at the age of 70.
The previous fall, just a few months before his diagnosis, the Tidwells and their daughter, Amy, took a family trip to Ireland. Judie graduated from Saint Mary’s College— the University of Notre Dame’s sister school— and wanted to watch the Fighting Irish play long-time rival, the Navy Midshipmen, in Dublin’s Emerald Isle Classic.
It was meant to be a trip filled with school spirit and adventure, but the mood was interrupted by Kenny’s unusual behavior.
“When we first got to Ireland, the first night in the hotel, he had no clue,” Judie said. “He was fumbling around and very discombobulated.”
Kenny wandered into the hallway of their hotel in the middle of the night several times, trying to get to the bathroom. He had trouble with money; he didn’t understand when to pay and when not to pay and struggled with basic math to calculate a tip. On the return home, Kenny tried to get on every flight that was boarding at the airport. Judie and Amy had to pull him back each time to make sure they didn’t lose him.
The two women returned to Houston in tears.
“The night we got home from Ireland, he said to my mom, ‘I think something’s wrong with me,’” Amy recalled. “In some ways, it was a relief because he had been fighting so hard for there to not be something wrong.”
Judie took Kenny to Baylor College of Medicine, where doctors diagnosed him with mild Alzheimer’s. Four years later, in 2017, his condition graduated to moderate Alzheimer’s.
“Most of the time, I understand, but I forget,” Kenny said. “It comes and it goes.”
The faces and places that colored Kenny’s memory are gradually fading. He’s aware that his memory is slipping and that trying to hold onto his past is like trying to grip sand in his hand. Try as he might to cling to what’s left, the sand will eventually trickle between the cracks of his fingers until his hands are empty.
“It makes me mad, frustrated, sad,” Kenny said. “It makes me want to cry.”

Judie and Kenny Tidwell go through their old wedding photos.
Learning from failure
Alzheimer’s is named for Alois Alzheimer, a German psychiatrist and neuropathologist who, in 1906, was the first to identify the neurodegenerative disease in a 55-year-old woman named Auguste Deter. Alzheimer studied Deter in a Frankfurt psychiatric facility for more than four years, until her death on April 8, 1906. He identified a host of unusual symptoms similar to dementia, including disorientation, loss of memory, unpredictable behavior and trouble with language.
After performing an autopsy, Alzheimer discovered high levels of a naturally-occurring protein in her brain. The clumps of amyloid plaques in Deter’s cerebral cortex (the part of the brain that controls personality, motor function, language and information processing), along with tendrils of tau proteins that had became entangled, disrupted normal communication between neurons in her brain. Today, Alzheimer’s disease is recognized as the most common form of dementia, although not everyone with dementia has Alzheimer’s.
Alzheimer’s disease has pillaged the memories, emotions, experiences, personalities and—ultimately—identities of millions of victims. To this day, it has no survivors.
The Alzheimer’s Association estimates that 5.8 million Americans are living with the disease; by 2050, this number is projected to reach nearly 14 million, with more baby boomers aging into a high risk of developing the disease. Because that risk increases with age, nearly one in two baby boomers who reach 85 will develop Alzheimer’s.
The disease progresses in three main stages: mild (early), moderate (middle) and severe (late).
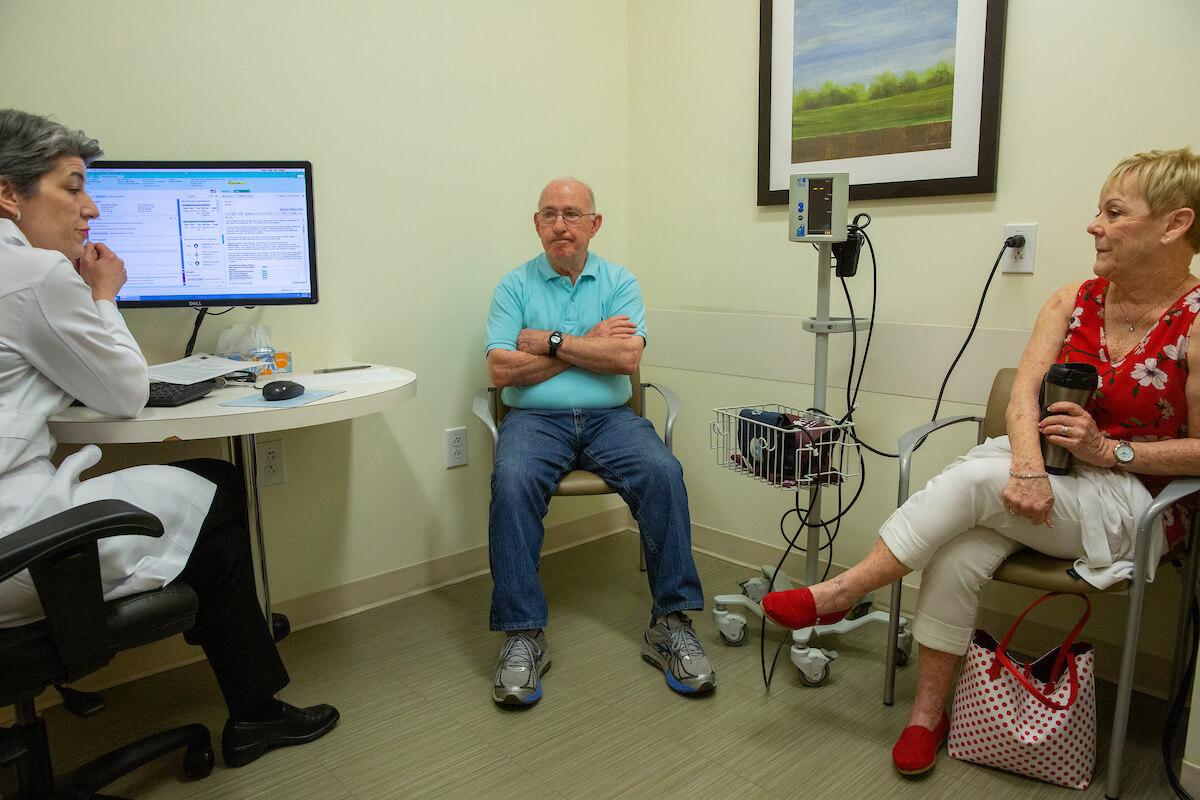
“The most common early presentation are things like disorientation, forgetting what day it is, repeating oneself, losing items within your home and not being able to retrace your steps,” said Melissa Michelle Yu, M.D., associate director of the Alzheimer’s Disease and Memory Disorders Center at Baylor College of Medicine. “There are normal things that happen with aging—we all forget our keys on the counter, those kinds of things—but … you go out the door without your keys and they’re in the refrigerator, that’s something different.”

Melissa Michelle Yu, M.D., associate director of the Alzheimer’s Disease and Memory Disorders Center at Baylor College of Medicine, tests Kenny’s vision.
More than a century after Alois Alzheimer characterized the disease, medical experts still don’t know what exactly causes it, how to prevent it and—most significantly—how to treat it. In pursuit of a cure, Alzheimer’s research has suffered scores of disappointments and dead ends. No drug exists to slow the progression of the disease. Instead, the Alzheimer’s medications currently on the market only treat symptoms. Cholinesterase inhibitors, for example, are used to control some behaviors associated with mild to moderate Alzheimer’s by preventing the breakdown of a chemical messenger in the brain.
The U.S. Food and Drug Administration (FDA) has not approved a new drug for the disease in more than a decade. The last FDA-approved therapy was Namenda—also known by its generic name, memantine—which is used to improve memory, awareness and daily functioning. That was 16 years ago. (In 2014, the FDA green-lit Namzaric, which is a combination of two long-approved Alzheimer’s drugs, memantine and donepezil.)
Most recently, in March 2019, Biogen halted two major studies on its drug, aducanumab, which was supposed to slow the progression of Alzheimer’s by targeting amyloids (proteins) long thought to destroy brain tissue. The drug showed great promise, according to data that Biogen and Japanese pharmaceutical partner Eisai presented at the Alzheimer’s Association International Conference in 2018. But no drug in history that specifically targeted amyloids has ever succeeded in defeating the scourge of toxic proteins responsible for Alzheimer’s—let alone keeping them at bay. In the end, Biogen’s promising drug was no exception.
But the lack of a cure is not for lack of trying.
“We learn from every failure,” Yu said. “Walking these patients and their families through the disease is difficult. It’s a difficult road they have to go down and I wish we had more that we could offer, but we’re learning more and more about what leads up to when the patient shows symptoms.”
Multifaceted problem, multidisciplinary solution
One of the most exciting developments in Alzheimer’s research has been identifying biomarkers in the brain, blood, urine and cerebrospinal fluid proteins that detect the disease before symptoms manifest. Currently, Alzheimer’s patients are diagnosed based on signs and symptoms of cognitive decline, but by that point, the disease has already been destroying brain tissue for decades.
“Identifying the Alzheimer’s pathology years before the onset of the clinical symptoms is really a huge advancement,” said Eliezer Masliah, M.D., director of the Division of Neuroscience at the National Institute on Aging (NIA).
Researchers are also working on developing vaccines to prevent Alzheimer’s. At the University of New Mexico, scientists recently engineered a drug using virus-like particles that eliminate tau tangles in mouse models. At Harvard Medical School, Cynthia A. Lemere, Ph.D., is working on an amyloid-targeting vaccine to prevent the disease.
However, because the scientific community has not yet reached a consensus on the precise pathology and causes of Alzheimer’s, it’s unlikely that a vaccine will become a reality anytime soon, said Jim Ray, Ph.D., head of the Neurodegeneration Consortium at The University of Texas MD Anderson Cancer Center’s Institute for Applied Cancer Science.
Instead of searching for a vaccine, Ray and his lab are working on a number of drug discovery projects focused on neuroinflammation and promoting a beneficial immune response in the brain.
“The brain has its own private immune system, separate from the blood-borne system that protects the rest of the body, and the cells that safeguard the brain are called microglia,” Ray explained. “As we have begun to understand what genes lead Alzheimer’s to run in families, we have identified a whole new slate of genetic risk factors. These new genes almost entirely map onto the microglia of the brain. We’re learning that the microglia reaction to the aging of the brain must be appropriate or there is a risk that Alzheimer’s pathology will take hold and begin to spread.”
In addition to genetics, a growing body of Alzheimer’s research has shown that lifestyle factors—physical, social and mental activity—may play a key role in reducing the risk of cognitive decline.
“One of the reasons we’re looking at lifestyle changes is because Alzheimer’s disease occurs over a continuum,” said Ann Marie McDonald, chief programs officer at the Alzheimer’s Association Houston & Southeast Texas Chapter. “Because of the use of PET imaging and things like that, we can start seeing those changes much earlier … and maybe we can intervene with lifestyle changes and be able to affect the disease progression. … Having to attack the disease from all fronts is really important.”
Because Alzheimer’s is a multifaceted problem that requires a multidisciplinary solution, collaboration is critical. “It’s not going to be one individual in one lab making a serendipitous finding,” Masliah said. “It is very similar to what you see now in the world of physics. To discover the Higgs boson, or to discover gravitational waves, it is not one individual working in one lab. It’s hundreds of individuals working together and making the data publicly available. I think we’re doing the same thing, and I think we’re beginning to see the products of this.”
Even if a cure is discovered today, it could take 10 to 15 years for drug therapy to make its way from the laboratory to the patient.
The caregiver
Because Alzheimer’s is a slowly progressing disease, life doesn’t stop the day of a diagnosis. It’s a very gradual goodbye.
“It hurt Kenny in the beginning to think that he’s losing [his memories], but after you reach a certain point, there’s no pain involved,” Judie said.
With Alzheimer’s, the family and friends closest to the patient may feel the pain of the disease the most.

Judie sits next to Kenny as he paints at Memory Café, a monthly social event for people living with Alzheimer’s and their loved ones.
Amy has watched the slow change in her parents’ relationship and witnessed the burden it places on her mother.
“She sees moments of their life together slipping away,” Amy said. “And they are.”
Because that shift from spouse to caregiver takes an emotional, mental and physical toll, support for Alzheimer’s caregivers is as important as support for patients.
“Over time, it’s always going to be a challenge as you lose that partnership—that true partnership—and that’s where the grieving comes in,” said Mary Kenan, Psy.D., a psychologist at the Alzheimer’s Disease and Memory Disorders Center at Baylor. “It’s not like a light switch. You don’t go to bed one day a spouse and, the next day, you wake up a caregiver. It’s that gradual transition.”
When Kenny was diagnosed, Judie joined a local Alzheimer’s support group that meets the second Monday of every month at the Good Shepherd Episcopal Church in Kingwood. For 90 minutes, it’s a brief respite for the husbands, wives, sons and daughters of Alzheimer’s patients.
“This is a place for ‘mekon hanekhama,’” said Barbara Hemphill, who started the group 17 years ago. “A safe place to do the work of grief.”
Last fall, Judie sat in a circle with 14 people in a small classroom at the church. The laughter that welcomed guests in the beginning died down as the jovial atmosphere became punctuated by somber moments, as each guest confronted the lonely reality of being an Alzheimer’s caregiver.
“He went to sleep,” said a woman in the support group, whose husband has severe Alzheimer’s. “A couple hours later, he woke up and made this sound like an animal. It was not human. Maybe he was dreaming, maybe he had a nightmare. I tell him, ‘Wake up, wake up,’ thinking he had a bad dream—and that’s when he spit on me. The sound he was making was awful. I went into the kitchen. We had a bottle of wine on the counter. He grabbed the bottle of wine and said, ‘I’m going to kill you.’”
A few people around the circle gasped. Others shook their heads in solemn understanding.
“I tried to get the bottle, but he was trying to get it away from me and smashed it on the counter,” she continued. “I tried to talk to him slowly, and we walked around the house, the both of us holding the bottle of wine. We walked, I don’t know, for what seemed to be hours, but it wasn’t, I’m sure. … He calmed down and went back to sleep.”
As Judie listened to the woman, she couldn’t help but feel thankful that Kenny is still as good-natured as he was before Alzheimer’s and remains mostly capable of taking care of himself—although now he struggles to find words and form sentences.
Members of the support group help Judie understand where this Alzheimer’s road is leading.
“They also show me how blessed we are that we are traveling said road so slowly,” she said.
But her mind is constantly fighting with her heart. She still loves Kenny the same way she has always loved him, but it’s heartbreaking watching him fade away.

The Tidwells share a light moment at home.
“Our anniversary was a rough day,” Judie said. Judie took Kenny out to a local steakhouse for dinner to celebrate their 43rd anniversary on Oct. 24.
She always loved spending their anniversaries together, but ever since Kenny developed Alzheimer’s, these celebrations have retained only the basic outline of anniversaries past. Kenny still prefers his steak cooked medium, but the significance of the date is lost on him. For him, Oct. 24 is just another day. Judie tries to find comfort in humor.
“You either laugh or you cry,” she said. “I try to make light of the situation because the alternative is crying yourself to sleep on your anniversary night.”
A matter of when, not if
Before Alzheimer’s, Kenny always had cheesy dad jokes and zingy one-liners at the ready.
Now, he is a little more subdued and disengaged.
“This new self is timid, unsure,” Amy said, adding that her father seems more comfortable around people he doesn’t know. “One time, my husband and I were daddysitting him. We took him to MOD Pizza. By the time we got to the counter, he was friends with everyone in the line. I think it’s because he doesn’t have to be self-conscious. They don’t know he has Alzheimer’s.”
The last time Amy caught a glimpse of the dad she grew up with was the day of her wedding, May 13, 2017.
“There was a part of him—the spark—that was back that I hadn’t seen in a long time. It was just like having him back for that day, and it was the perfect day for him to make an appearance,” Amy recalled. “Even now, sometimes he just comes out and you’re just like, ‘There he is!’ Then you blink and he’s fading away again.”
Barring any other health issues, Kenny’s condition will progressively worsen as he advances into late-stage Alzheimer’s.
As more faces and memories evaporate from his mind, he’ll also lose the ability to eat, speak and walk.
“Once they cross that plane, they’re not hurting anymore,” Judie said. “They’re not upset by it. They don’t know the difference. It hurts the people who are watching it.”
Judie tries not to think that far into the future. She has prepared by purchasing a long-term care insurance policy, but there’s little she can do to ease the fear of not being able to look after her husband.
“I think mostly about what will happen when I can no longer take care of him,” Judie said. “Where would I put him?”
Amy has watched the disease erode her father’s mind and identity for years.

Kenny Tidwell walks up the stairs in his Kingwood, Texas, home.
“I worry about him, but I worry about her more because I know how hard it’s going to be for her,” Amy lamented.
“I think it’s worse when he’s going to be cognizant less and less, and she’s going to be lonelier and working harder trying to keep him at home.”
For the past few years, Judie and Amy have talked about the day Kenny will no longer recognize them. They have always known it’s not a matter of if it will happen—it’s a matter of when. This spring, Amy’s greatest fear came true. On the way home from Easter brunch, Kenny turned to Judie and asked if Amy was his sister.
“I was devastated,” said Amy, who was riding in the car with her parents and overheard her father’s question. “It was just like someone had punched me in the stomach. All I could think was, ‘I thought I had more time.’”
‘Something someone can do right now’ One major problem in Alzheimer’s research is the low rate of participation in clinical trials, Masliah said.
Kenny has participated in clinical trials through Baylor, including one in 2017 that tested BACE (beta-site amyloid precursor protein cleaving enzyme) inhibitor drug verubescestat. Although that drug ultimately joined the mass of other failed drugs, Kenny’s participation—along with that of other affected patients— was essential.
“We want to help, but we need their help, as well,” Masliah said. “The progress is not only thanks to what people are doing in their labs, but really it’s thanks to them. To test these drugs, [patients] need to participate in clinical trials.”
The NIA is currently ramping up efforts to recruit more patients for various Alzheimer’s studies, including two types of prevention trials: one in which the disease pathology is already present but patients show no clinical symptoms, and another in which individuals show no pathology and no clinical symptoms.
Studying both affected and healthy individuals is critical to Alzheimer’s research, but it’s a tough sell.
“It’s the same thing with many other diseases: people get into a clinical trial when they have a very advanced disease and they are motivated,” Masliah said. “When you ask people to participate in a clinical study … when they are clinically healthy, it’s harder.”
While reports of failed studies may be disheartening, experts urge people not to lose hope in clinical trials.
“If you want to be part of a solution,” McDonald said, “this is something someone can do right now.”
‘Right now’ is where Judie tries to keep her heart and her head. For the moment, she is Kenny’s memory, his link with a rich and happy past. She is there to answer his same questions, over and over again.
“He just wants to know when he’s going to get better,” Judie said. “I say, ‘Kenny, you’re not going to be better. The goal is to keep it moving slowly like it is right now.’ Then he forgets he asked.”

The Tidwells in 2019.