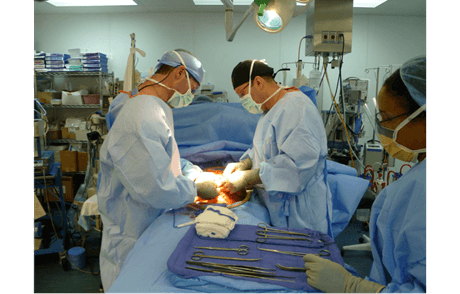
On the front lines of health care

Veterans Day, observed every November 11, honors the men and women of the U.S. Army, Navy, Air Force, Marine Corps and Coast Guard. TMC Pulse asked several veterans who work at the Texas Medical Center how their military training has helped them serve the world’s largest medical city.
……………………………………………………………………………………………………..
JOYCE BURNS: Associate Director of the Stroke Program and family nurse practitioner at the Michael E. DeBakey VA Medical Center Houston; retired lieutenant colonel in the U.S. Army
When Joyce Burns was a girl, home health nurses came by regularly to check on her ailing grandmother.
“All of the nurses used to tell me what they were doing for my grandmother—putting in catheters, caring for wounds—and it seemed like a very interesting career,” Burns said.
Because of a chance encounter, Burns decided to join the army while she trained to become a nurse.
“One day my high school announced that there were two army recruiters in the cafeteria. One of my friends and I, we were in homeroom and we were looking for a way to slip out, so we went down to see their presentation,” she said. “My mom wasn’t too excited because back in the ’70s there weren’t as many women in the military, but I really wanted to go and my dad was very supportive.”
Burns served in the U.S. Army for 26 years before retiring as a lieutenant colonel in 2003. She received her bachelor’s in nursing from the University of South Carolina and her masters from the United States Army War College. She worked at army hospitals in Texas, South Carolina, California, Georgia and Colorado.
Today, Burns serves as Associate Director of the Stroke Program and a family nurse practitioner on the neurology care line at the Michael E. DeBakey VA Medical Center Houston.
“One of things I learned and carry with me today is that the military is like a family,” Burns said. “It is similar here at the VA because we are like a family. With the patients that I am taking care of,
I think about the time that they have put in. In the military you are moving around and your kids aren’t able to be raised near family, so on active duty you build a camaraderie.”
……………………………………………………………………………………………………..
JOSEPH LOVE, M.D.: Medical Director of Memorial Hermann Life Flight, director of the General Surgery Residency Program and associate professor at McGovern Medical School at UTHealth ; retired lieutenant colonel in the U.S. Air Force
Growing up in Fairbanks, Alaska, Joseph Love didn’t anticipate he would have a career in the military or in medicine. But after completing his master’s degree, his wife convinced him to apply to medical school.
“We applied all over the place and I got in, and as a young couple, now that we’ve done this, the question was, how do we pay for it?” Love said. “The military has something called a Health Professions Scholarship Program. I applied for it and got it, so they paid all my tuition, they bought all my books and supplies. And then, in return, you have to give back one year for every year that you are in medical school.”
Over an eight-month period starting in 2010, Love was deployed to Bagram Airfield in Afghanistan during a very volatile period. While there, Love operated on U.S. soldiers and civilians. He was also known around the base for slipping a few Girl Scout Cookies under the pillows of his patients—not only to give them a treat from home, but also to remind them of U.S. programs that empower young women.
When Love made it back state-side, he accepted a job at Life Flight working under founder James “Red” Duke, Jr., M.D.
“I don’t think I’d have the job I do if I hadn’t had those experiences. I’m a small-town kid. I’m not boisterous,” Love said. “My early discussions about Afghanistan with Red Duke … He was there before the wars and he started up the medical school in Kabul. Although our experiences were vastly different—his memories of Afghanistan were a little bit romanticized compared to my experience—that sort of kindred relationship let him and my relationship grow to the point where he trusted me enough to take over Life Flight as the medical director.”
In addition, the trauma Love saw in Afghanistan prepared him to care for Life Flight patients.
“I came here in 2011, just a few years out of fellowship, but the volume of trauma and breadth of trauma that I saw on the military side—it would take years to see that here,” Love said.
……………………………………………………………………………………………………..
PATRICIA DARNAUER: Senior Vice President of Support Services at Harris Health System; retired colonel in the U.S. Army Medical Service Corps
In Afghanistan, Patricia Darnauer commanded a combat support hospital—a deployable medical task force.
“We were down in Helmand province. In 2011, that was a pretty hostile environment; we supported marines and we were a trauma hospital,” Darnauer said. “It was an amazing time to know that you could make a difference. The one incredibly positive thing about a deployment is that sense of unity focus—everyone was there to take care of the soldier, the sailor, the civilian that came in—and Afghan soldiers.”

Just over two years ago, Darnauer accepted the position of Senior Vice President of Support Services at Harris Health System.
“The military teaches you to grow and to be a leader, to accept responsibilities and to be flexible,” she said. “All of those things translate into the civilian sector. If there was one thing that transferred over without a second thought it was that mission focus—taking care of your patient, taking care of that population. Many of our patients, truth be told, they don’t have many advantages or options in their lives, so to know that we are an entire health system that is focused on taking care of them and bringing them the best care possible is really meaningful and important.”
……………………………………………………………………………………………………..
GEORGE V. MASI: President and CEO of Harris Health System; retired colonel in the U.S. Army Medical Service Corps
When George V. Masi joined the U.S. Army in 1973 as an officer in the Medical Service Corps, he didn’t plan to spend more than two years on active duty. But one tour turned into two, and that turned into a 27-year career that took Masi and his family to Korea, Germany and several different locations in the United States.
Before coming to work at Harris Health, the largest safety-net health care system in the region, Masi worked with Ben Taub Hospital— one of the institutions within Harris Health System.
“The army, navy and air force used to send their surgeons to Ben Taub Hospital to a facility called the Joint Trauma Training Center,” Masi said. “There was no war and the military needed a place to have their trauma surgeons train and Ben Taub was that hospital.”
Masi has been with Harris Health for 17 years, but still brings lessons learned from the army to work with him every day.
“In the army, we used to say, ‘Take care of the soldiers and they will take care of you if you are a leader,’ and the same holds true in the civilian sector,” Masi said. “So much of it is about people—treating people with dignity and respect, knowing full well that the mission is difficult. … If you are attentive to the needs of your people—whether they are soldiers or, in this case, civilian members of the team—they will do incredibly wonderful things. That was my experience in the military and it has been my rewarding experience here at Harris Health.”
……………………………………………………………………………………………………..
YONG CHOI, M.D.: Bariatric surgeon at CHI St. Luke’s Health-The Woodlands Hospital; retired colonel in the U.S. Army
During a 25-year career in the military, Yong Choi, M.D., was deployed to the Middle East four times.
“I was deployed to Kuwait on Thanksgiving Day 2001 and then subsequently deployed … once to Iraq and two more times to Afghanistan,” Choi said. “While over there, we cared for U.S. and allied soldiers, local nationals, civilians and prisoners if they needed medical treatment. I can’t think of anything better than taking care of the soldiers in the military. They are the best patients and they are so grateful.”
A Houston native, Choi graduated from the U.S. Military Academy (West Point) before beginning his medical career with the armed forces. He completed medical school at the Uniformed Services University of the Health Sciences in Bethesda, Maryland; residency at Eisenhower Army Medical Center in Augusta, Georgia; did a fellowship in general surgery at Baylor College of Medicine and then became a general surgeon in the U.S. Army.
Upon retiring from the army last year, Choi began working as a bariatric surgeon at CHI St. Luke’s in the Woodlands. He uses many of the skills he learned in the military in the operating room.
“The best thing that I learned in the service was time management and teamwork,” Choi said. “What you see out there and everything that happens in the military, it doesn’t happen with one person by themselves. It requires a lot of effort, teamwork, cooperation and attention to detail. That also relates to medicine. Especially in my field as a surgeon, it is very important to make sure you don’t deviate from how you do things and you do the same thing over and over and have a really keen attention to detail. I see the OR as just a big team operating—there’s anesthesia personnel, circulating nurse, scrub nurse and you all have to be on the same page and no one person is more important than anyone else. Everyone is just as integral to the team.”
……………………………………………………………………………………………………..
ROBERT ATHEY: McGovern Medical School student; retired sergeant in the U.S. Marine Corps
Robert Athey, a first-year student at The University of Texas Health Science Center at Houston’s McGovern Medical School, decided to become a doctor while serving in the U.S. Marine Corps in Afghanistan.
“I ended up deploying to Afghanistan in 2012,” Athey said. “The unit I was in was more medical related stuff—almost like what an EMT does.”
During his deployment, Athey provided care for U.S. soldiers, Afghan soldiers and civilians.
“The whole local population there didn’t really have access to care other than the Marines. We were the ones they would come to for pain medication if someone was hurt or sick,” he said. “There were mixed emotions because sometimes you were providing care to people who actually wanted to do harm to you because that is how the Geneva Convention works. But you put yourself aside in that moment and try to alleviate symptoms the best you can.”
After five years in the Marine Corps, Athey returned home and attended Baylor University in Waco, Texas, before being accepted to McGovern Medical School.
“I look back at my years in high school and I wasn’t well disciplined and I couldn’t apply myself to school very well,” Athey said. “In the Marine Corps, I went in as an intelligence analyst—it is a very school-intensive job and they retaught a lot of study skills I needed. I ended up growing in maturity in the military and it has helped me achieve my goals—for example, getting into medical school.”